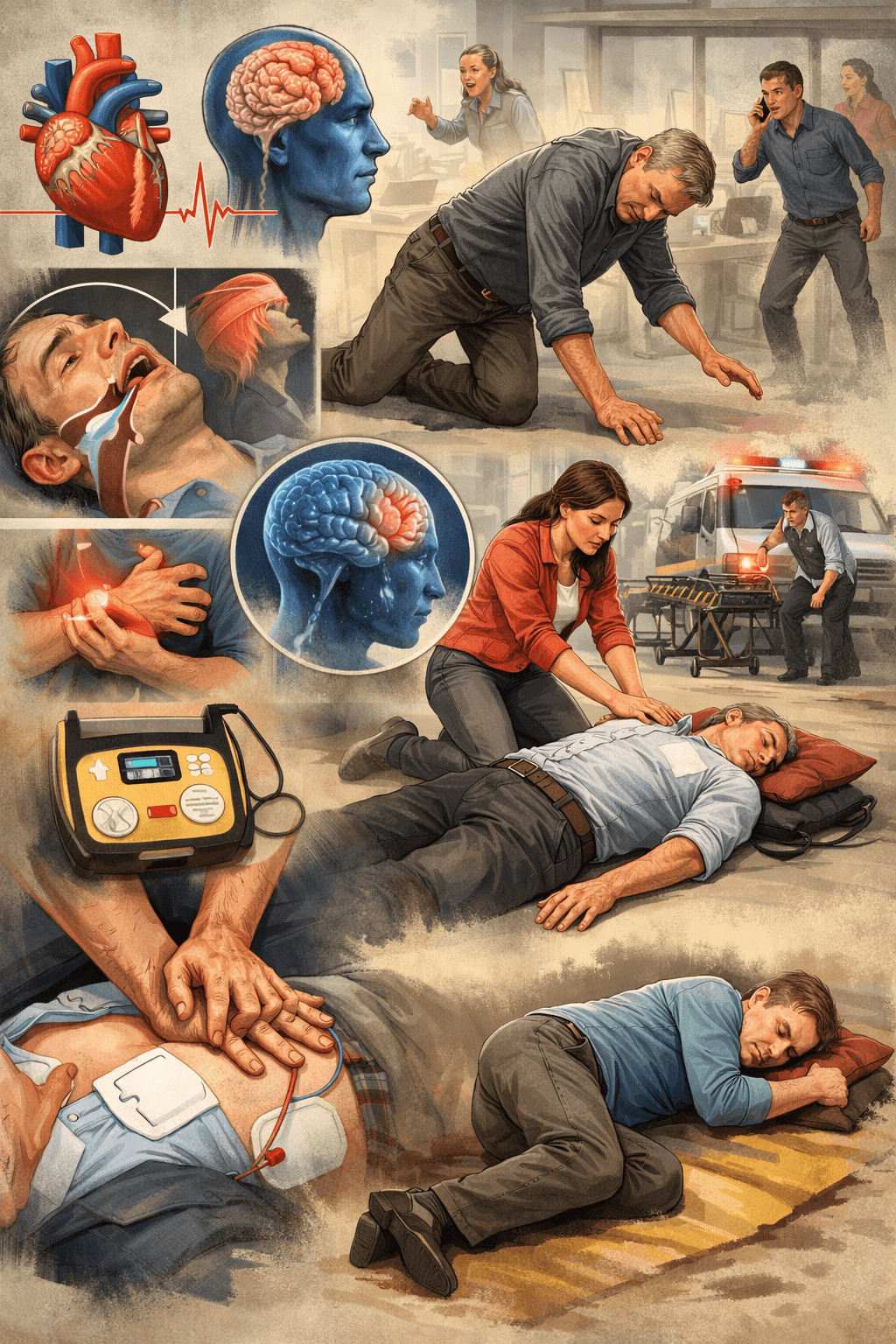
Sudden collapse refers to a situation where a person suddenly loses consciousness and falls, often without clear warning signs. This can occur at home, in the workplace, or in public settings, and must always be treated as a medical emergency requiring immediate recognition and response.
Possible Causes of Sudden Collapse
- Cardiac arrest
- Myocardial infarction (heart attack)
- Stroke
- Seizure
- Severe hypoglycemia
- Syncope (fainting)
In many situations, bystanders cannot determine the exact cause. Therefore, the priority is to rapidly assess vital status and activate emergency medical services (EMS).
Key Pathophysiological Risks
1. Cardiac Arrest
Cardiac arrest occurs when the heart stops pumping effectively, leading to:
- Circulatory arrest
- Rapid cerebral hypoxia (lack of oxygen to the brain)
Irreversible brain injury may begin within 4–6 minutes without oxygen if resuscitation is not initiated. This is one of the most life-threatening causes of sudden collapse.
2. Airway Obstruction
In an unconscious person:
- Protective airway reflexes are reduced
- The tongue may fall backward and block the airway
- Risk of aspiration (vomit or secretions) increases
Maintaining a clear airway is a top priority.
3. Cerebral Hypoxia
When breathing or circulation is impaired:
- The brain does not receive adequate oxygen
- Brain cells begin to deteriorate rapidly
Early intervention directly impacts neurological recovery.
4. Syncope (Fainting)
Not all collapses are due to cardiac arrest. Syncope occurs due to temporary reduction in blood flow to the brain, commonly caused by:
- Low blood pressure
- Dehydration
- Prolonged standing
- Cardiac arrhythmias
The person may regain consciousness within minutes, but medical evaluation is still recommended if the cause is unclear.
5. Seizure
Seizures may cause:
- Sudden loss of consciousness
- Muscle stiffness and jerking
- Uncontrolled collapse
Main risks include:
- Injury from falling
- Airway obstruction
- Aspiration during the post-seizure phase
Do NOT restrain the person or place objects in their mouth.
6. Other Causes
- Hypoglycemia
- Stroke
- Electrolyte imbalance
- Intoxication or excessive alcohol use
- Medication side effects
In real-life situations, do not delay care trying to identify the exact cause. Focus on assessment and immediate response using the ABC approach.
Common Mistakes
- Not checking the victim’s condition
- Forcing the person to sit or stand
- Splashing water or slapping the face
- Giving food, drinks, or medication
- Assuming the person is “just tired” or has “low blood pressure”
These actions may delay recognition of a life-threatening emergency.
Initial Assessment – ABC Approach
A – Airway
Check if the airway is open. Obstruction may be caused by:
- Tongue falling backward
- Foreign objects
- Vomit, blood, or secretions
If the airway is blocked, oxygen cannot reach the lungs.
B – Breathing
Look for normal breathing for no more than 10 seconds:
- Observe chest movement
- Assess whether breathing is regular and effective
Agonal breathing (gasping) is NOT normal breathing.
C – Circulation
Check for signs of circulation, such as:
- Movement
- Normal breathing
- Responsiveness
Also observe:
- Pale or bluish skin
- Severe bleeding
If the person is unresponsive and not breathing normally → suspect cardiac arrest.
When to Call Emergency Services Immediately
- Unresponsive
- Not breathing or abnormal breathing
- Seizure activity
- Chest pain before collapse
- Weakness or paralysis
- Head injury
Even if the person regains consciousness, medical evaluation is still required.
Key Response Priorities
- Assess consciousness
- Check breathing
- Activate EMS early
- Start CPR when indicated
Initial First Aid Management
1. Ensure Scene Safety
- Check surroundings
- Remove potential hazards
2. Check Responsiveness
- Call out loudly
- Gently tap the shoulders
If no response → treat as an emergency.
3. Check Breathing
Look for normal breathing for no more than 10 seconds
4. Activate Emergency Medical Services (EMS)
Call for help as early as possible. Early intervention significantly improves survival.
5. Start Cardiopulmonary Resuscitation (CPR) if Needed
If the person:
- Is unresponsive, AND
- Is not breathing or not breathing normally
Start chest compressions immediately (if trained) and if an Automated External Defibrillator (AED) is available:
- Retrieve it
- Follow voice instructions
If the Person is Unconscious but Breathing
- Place in the recovery position (on their side)
- Monitor breathing continuously
- Wait for Emergency Medical Services
This helps prevent:
- Airway obstruction
- Aspiration
Immediate and appropriate action in the first few minutes can determine survival and the extent of brain injury.